
Standard 2.9: Don't Let Workforce Failure Become a Reputational Crisis.
As Used & Trusted
If you miss Standard 2.9, it won’t just be a red mark in an audit – it’s the kind of failure that shows up in coroners’ reports, media headlines and emergency board meetings.
Right now, every weakness in your workforce – a missed police check, a thin evening skill mix, a rushed induction, a supervisor who “keeps an eye on things” but never documents performance – is a risk you are carrying personally as an executive or board member. Regulators won’t ask whether you have policies; they’ll ask why an unvetted, poorly trained worker was left alone with vulnerable residents when something went wrong.
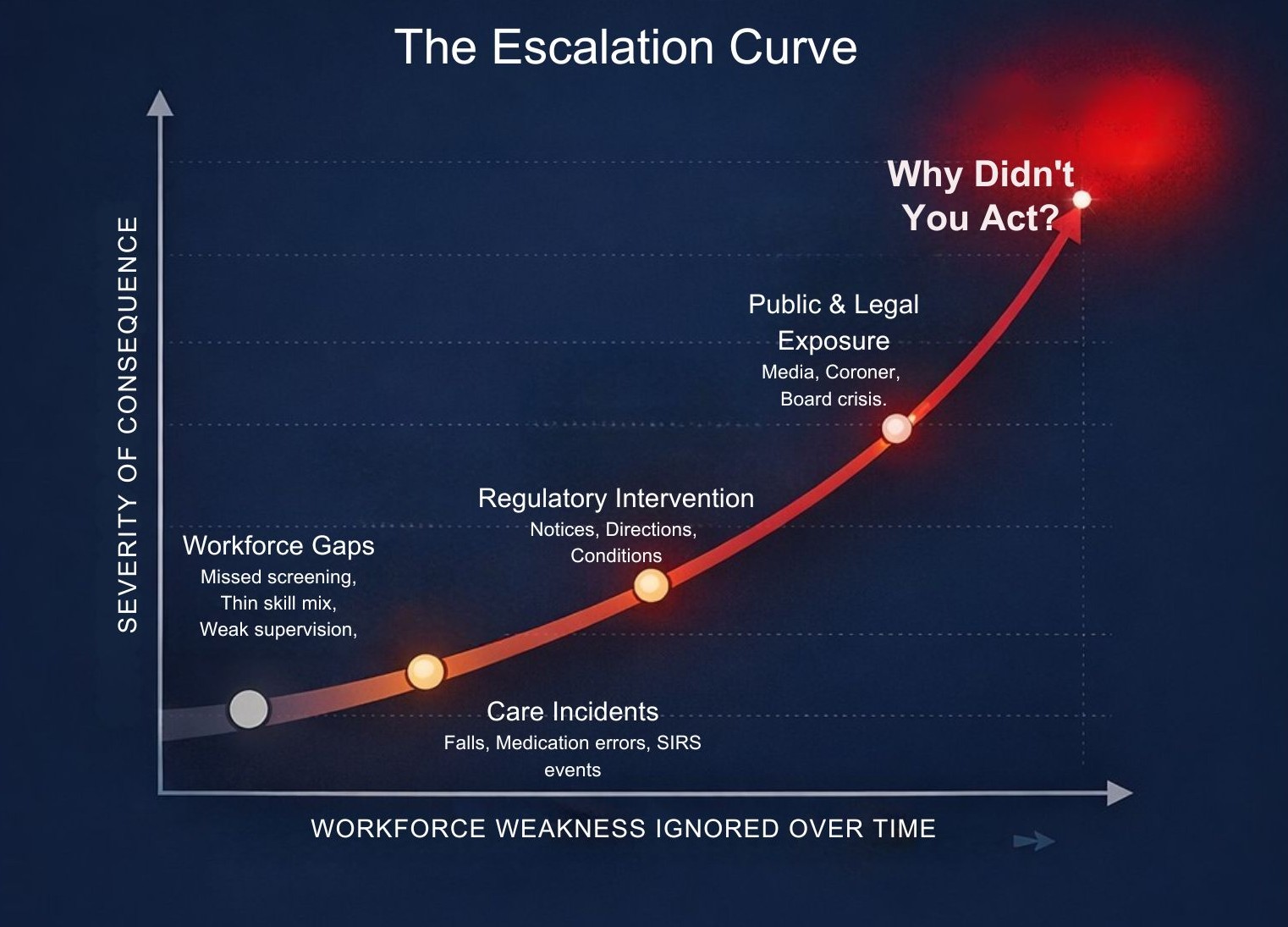
When Standard 2.9 is not under control, three things tend to happen.
First, older people get hurt. Medication mistakes, missed deterioration, rough or disrespectful care, poor responses to behaviours or emergencies – these are not abstract risks, they are exactly what you see when inexperienced, unsupported staff are rostered into complex shifts without the right skill mix or supervision. One bad shift, one preventable fall, one mis‑managed incident can become a Serious Incident Response Scheme notification, a complaint to the Commission, and a family demanding to know why their parent was not safe.
Second, your workforce starts to fracture. Good staff burn out covering unsafe rosters. Weak performers are never confronted because performance reviews are a tick‑box exercise. Training becomes a sign‑in sheet instead of proof of competence. Over time, you’re left with a revolving door of agency staff and new starters who don’t know your residents, your systems, or your expectations – but they are still the ones making minute‑to‑minute decisions about care.
Third, the regulator steps in – and they will join the dots. A failure against 2.9 doesn’t sit neatly in one box; it bleeds into governance, clinical care, incidents and complaints. Once the Commission sees a pattern – repeated SIRS events with workforce elements, skill mix issues on critical shifts, patchy screening records, vague supervision arrangements – they have everything they need to move from “recommendations” to “directions”, conditions on your approval, restrictions on admissions or, in the worst case, the end of your business as an aged care provider.
This is why treating Standard 2.9 as “an HR thing” is dangerous. If you can’t, on any given day, show exactly who is on the floor, how you know they are screened, competent, supervised and reviewed – and how you are actively managing the workforce risks that keep your executives and board awake at night – then you are effectively hoping that nothing goes wrong. Hope is not a defence in an audit, and it is never an answer when a family, a regulator or a coroner asks: “You knew these workforce risks existed. Why didn’t you act?”
Blog Related
The 5-Minute Mentor: Aged Care Learning Insights
Transform your aged care team with monthly microlearning insights you can implement immediately.






